October 19, 2022 -- Virginia Tech researchers have discovered that infection with a bacterium causes pancreatic cells to release cytokines that promote solid tumor growth, potentially helping to guide future therapeutic interventions for cancer treatment.
Their study, published October 18 in the journal Science Signaling, found ways in which the bacterium may directly impact cancer progression and resistance to chemotherapy treatments.
Earlier research found a correlation between high intratumoral loads of Fusobacterium nucleatum and shorter survival in patients with pancreatic ductal adenocarcinoma (PDAC). The finding is part of a body of evidence that implicates the tumor microbiome in cancer progression and resistance to chemotherapy. However, the mechanism through which F. nucleatum promotes PDAC was unknown.
To shed light on the mechanism, researchers at Virginia Tech studied how various subspecies of the bacterium interact with human PDAC cell lines and normal human pancreatic epithelial cells. The team found that F. nucleatum causes both cell types to secrete increased amounts of the cytokines GM-CSF, CXCL1, IL-8, and MIP-3α.
The cytokines increased proliferation, migration, and invasive cell motility in infected and noninfected PDAC cells, but not in noncancerous pancreatic epithelial cells. The researchers suggested autocrine and paracrine signaling to PDAC cells as a potential explanation for the different responses of the healthy and cancerous cells. PDAC cells proliferated in the presence of all tested strains of F. nucleatum, regardless of whether immune and other stromal cells were present.
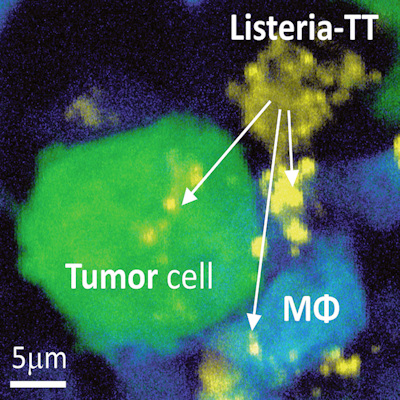
Those findings were made possible by in vitro tumor-on-a-chip models. The models confirmed that the bacterium can bind and invade the pancreatic cancer cells, causing them to secrete molecules that drive their proliferation. Using the models to generate those insights explained why the researchers saw more migrated pancreatic cancer cells than they expected during their initial analyses of cell migration.
Introducing an antibody to block GM-CSF signaling "markedly limited proliferative gains after infection," the researchers found. The effect of the antibody supports the potential for knowledge of interactions between the host and tumor microbiome to inform therapeutic interventions. However, the team still has work to do to translate the findings into humans, as Scott Verbridge, associate professor in biomedical engineering and mechanics at Virginia Tech, explained.
"While we have shown that F. nucleatum is capable of driving pancreatic cancer cell proliferation and migration, we do not yet know to what extent these outcomes translate to living systems or human patients. These next steps will be important future work, which could ultimately teach us whether or not this knowledge could lead to more effective therapies that are tailored to a patient's own microbiome components," Verbridge, a co-author of the paper, said in a statement.
Copyright © 2022 scienceboard.net