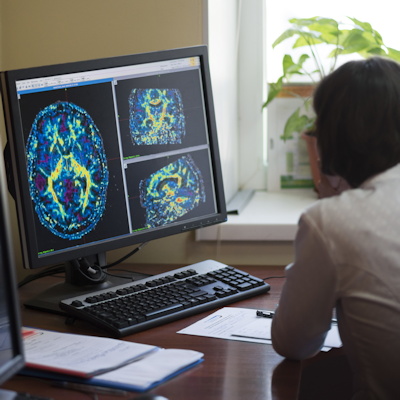
March 2, 2023 -- Piggybacking on the homing mechanism that the immune system uses to direct white blood cells could enable the targeted delivery of drugs in children with brain tumors, according to research published on Thursday in Nature Materials.
Today, children with medulloblastoma, the most common pediatric brain tumor, receive chemotherapy and radiotherapy. The treatment has a five-year survival rate of more than 70%, but its side effects can leave children with long-term disabilities and health issues. As such, there is a need for treatments that are more effective and have better safety profiles.
Researchers at Mount Sinai Health System and Memorial Sloan Kettering Cancer Center think targeted drug delivery may address this unmet need. By directing therapies to the tumor, physicians could deliver higher doses to the affected tissues without harming healthy cells.
The blood-brain barrier, which controls which molecules enter the brain, makes it hard to achieve such targeting. However, the researchers identified a mechanism that could overcome the challenge. Proteins at inflammation sites serve as beacons for white blood cells, enabling targeted immune responses. Using these proteins, the scientists sought to send drug-loaded nanoparticles to target tissues.
In a mouse model, the approach enhanced the efficacy of an anticancer drug that could be beneficial to medulloblastoma patients but is held back by bone toxicity. The formulation, which was enhanced by the administration of very low-dose radiation, could get more of the drug to the brain and less to the bone, thereby make the risk-benefit profile more favorable.
"We show that we can more successfully deliver lower doses of the drug in a more effective manner to the specific sites of tumor within the brain, while sparing the bone toxicity that is seen in younger patients," Dr. Praveen Raju, PhD, co-director of the Children's Brain and Spinal Tumor Center at Mount Sinai Kravis Children's Hospital and senior author of the study, said in a statement.
The paper builds on earlier work Raju has been involved with. In 2020, the physician published research into the use of a Sonic Hedgehog (SHH) pathway inhibitor, vismodegib, packaged in a fucoidan-based nanoparticle in mice. SHH medulloblastoma accounts for around 25% of cases; clinical trials suggest that vismodegib may help some patients, although on-target bone toxicities are a problem.
By pairing vismodegib with a nanoparticle that targets P-selectin, a transmembrane protein expressed on epithelial cells, Raju and his collaborators enhanced mouse survival without causing the bone toxicity that is normally associated with the SHH pathway inhibitor.
Copyright © 2023 scienceboard.net