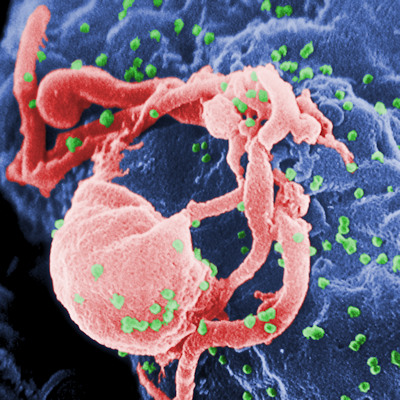
March 16, 2023 -- Transplanting stem cells from umbilical cord blood has potentially cured a mixed-race woman of HIV and freed her from taking antiviral medication, according to a case report published in Cell.
The individual, known only as the New York patient, is a middle-aged woman who self-identifies as mixed race. In 2017, the patient had leukemia and HIV. A team at Weill Cornell Medicine transplanted CCR5-delta32/32-carrying stem cells from banked umbilical cord blood to try to cure the cancer and HIV simultaneously.
The researchers have now published evidence that the treatment worked: the patient's HIV and cancer went into remission after the transplant. Approximately three years after the transplant, the patient stopped taking the antiviral medication she was using to keep the HIV virus under control. The patient has been HIV-negative for more than 30 months since she stopped taking the HIV antivirals, leading the physicians to present the transplant as a possible cure.
The New York patient is one of several people who have potentially been cured of HIV by stem-cell transplants. Since the successful treatment of the "Berlin patient" in 2009, two other men, in Düsseldorf and London, have undergone stem-cell transplants to eliminate the HIV virus. The case of the New York patient is different.
To treat the first three patients, physicians found donor cells from compatible adults carrying two copies of the CCR5-delta32 mutation. The presence of the CCR5-delta32 mutation is critical because it stops HIV from entering and infecting cells and thereby confers resistance to the virus. However, around 1% of white people have two copies of CCR5-delta32 and the mutation is even rarer in other groups.
The rarity of homozygous CCR5-delta32 mutations in people of color led the physicians treating the New York patient to conclude that it would be almost impossible to find a compatible adult donor. To work around this barrier to treatment, the physicians instead transplanted CCR5-delta32/32-carrying stem cells from banked umbilical-cord blood. The patient simultaneously received stem cells from a relative.
University of California, Los Angeles' Yvonne Bryson, who co-led the study with Johns Hopkins University School of Medicine's Deborah Persaud, explained the thinking behind the treatment in a statement.
"Using cord blood cells broadens the opportunities for people of diverse ancestry who are living with HIV and require a transplant for other diseases to attain cures," Bryson said. "With cord blood, you may not have as many cells, and it takes a little longer for them to populate the body after they're infused. Using a mixture of stem cells from a matched relative of the patient and cells from cord blood gives the cord blood cells a kick start."
While cord blood opens opportunities to treat more patients, using stem cells to cure HIV is likely to remain a rarity. Transplants are not used to treat HIV in isolation because they require the patient to undergo chemotherapy or radiation to eliminate their immune system. However, if a patient needs to undergo those treatments and receive a stem-cell transplant to treat their cancer, there is a chance to potentially cure HIV at the same time by using CCR5-delta32/32-carrying stem cells.
Copyright © 2023 scienceboard.net