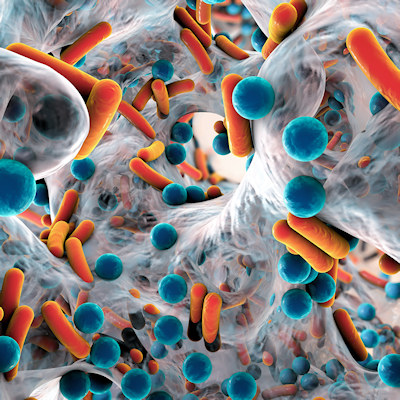
February 14, 2023 -- Two of the most dangerous multidrug-resistant pathogens work together to nullify antibiotics, suggesting physicians need to determine if both bacteria are present before selecting a treatment regimen.
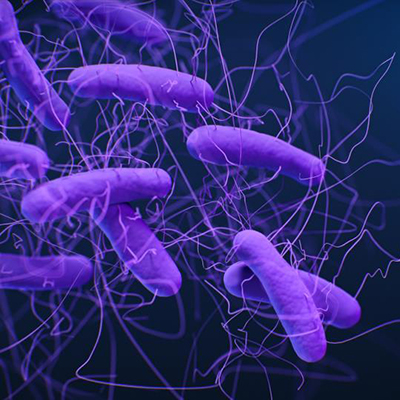
The study, details of which were published in Nature Communications, examined interactions between Acinetobacter baumannii and Klebsiella pneumoniae strains co-isolated from a human lung infection. A. baumannii is one of three pathogens that the World Health Organization sees as a critical priority. Both bacteria are part of the group of six highly virulent, resistant pathogens known by the acronym ESKAPE.
Using transcriptomic, phenomic, and phenotypic assays, researchers at Australia's Macquarie University and University of Newcastle sought to understand why dual infections with the bacteria are associated with increased antibiotic resistance and mortality rates.
Analysis of dual-species co-culture biofilms revealed that each bacteria helps the other. K. pneumoniae cross-feeds A. baumannii its byproducts of sugar fermentation, namely ethanol and lactate, and thereby supports the growth of the other pathogen. At the same time, A. baumannii releases enzymes that break certain antibiotics. The release of cephalosporinases enabled K. pneumoniae to tolerate higher levels of antibiotics than it can survive in the absence of A. baumannii.
The findings have implications for the diagnosis and treatment of infections with the two pathogens, as Macquarie University's Lucie Semenec explained in a statement. "This research is significant because diagnostic methods commonly look for the most dominant pathogen and therefore treatment is targeted at that," Semenec said. "New drugs now can be informed in future research by the molecular mechanisms we find in this work."
Only considering the predominant infecting microorganism when diagnosing bacterial infections enables physicians to focus treatment on the most prevalent, and therefore potentially the most problematic, pathogen. However, the work of Semenec and her collaborators suggests limiting the diagnosis to the predominant microorganism may result in suboptimal treatment.
If A. baumannii is predominant, its growth rate will vary depending on whether K. pneumoniae is present or not. Knowing that A. baumannii has a growth advantage could help optimize treatment. Similarly, the discovery of A. baumannii in a patient with a K. pneumoniae infection will reveal that the efficacy of cephalosporins such as cefotaxime may be reduced.
The two pathogens are both involved in a range of respiratory, urinary tract, and blood infections. By determining if both bacteria are present, physicians may be able to provide a more effective treatment and minimize the risk that cross-feeding and cross-protection will enable pathogenic biofilms to survive in the presence of high concentrations of antibiotics.
Copyright © 2023 scienceboard.net