October 27, 2022 -- As heart cells mature in mice, the number of communication pathways called nuclear pores dramatically decreases. While this might protect the organ from damaging signals, it could also prevent adult heart cells from regenerating, finds new study.
In the study published October 24 in the journal Developmental Cell, researchers from the University of Pittsburgh and University of Pittsburgh Medical Center (UPMC) provide an explanation for why adult heart cells do not regenerate themselves. They suggest that quieting communication between heart cells and their environment protects the organ from harmful signals related to stresses such as high blood pressure, but it prevents heart cells from receiving signals that promote regeneration.
"These findings are an important advance in fundamental understanding of how the heart develops with age and how it has evolved to cope with stress," Dr. Bernhard Kühn, director of the Pediatric Institute for Heart Regeneration and Therapeutics at Pitt School of Medicine and UPMC Children's Hospital of Pittsburgh, said in a statement.
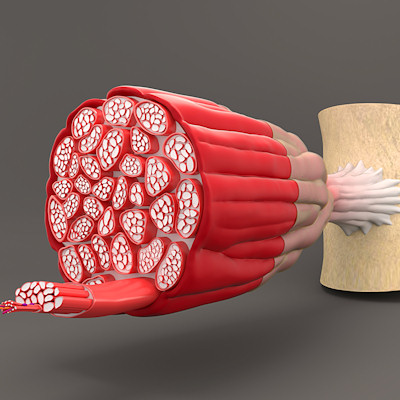
To help with this investigation, Kühn teamed up with fellow Pitt researchers and biomedical imaging experts Yang Liu, PhD, associate professor of medicine and bioengineering, and Donna Stolz, PhD, associate professor of cell biology and pathology and associate director of the Center for Biologic Imaging. They looked at nuclear pores -- perforations in the lipid membrane that surround a cell's DNA and regulate the passage of molecules to and from the nucleus.
Using super-resolution microscopy, Liu visualized and counted the number of nuclear pores in mouse heart cells, or cardiomyocytes. The number of pores decreased by 63% across development, from an average of 1,856 in fetal cells to 1,040 in infant cells to just 678 in adult cells. These findings were validated by Stolz who used electron microscopy to show that nuclear pore density decreased across heart cell development.
The study showed that blocking expression of a gene called Lamin b2 -- which is highly expressed in newborn mice but declines with age -- led to a decrease in nuclear pore numbers in mice; these mice had diminished transport of signaling proteins to the nucleus and decreased gene expression, suggesting that reduced communication with age may drive a decrease in cardiomyocyte regenerative capacity.
The researchers used a mouse model of high blood pressure to understand how nuclear pores contribute to structural remodeling of the heart, which is a major cause of heart failure. Mice that were engineered to express fewer nuclear pores showed less modulation of gene pathways involved in harmful cardiac remodeling. These mice also had better heart function and survival than their peers with more nuclear pores.
Copyright © 2022 scienceboard.net