May 5, 2020 -- A new study aims to further classify the immune response of COVID-19 patients with the goal of understanding the pathogenesis of the disease and accelerating the development of an effective vaccine to SARS-CoV-2 infection. The results of the study were published in Immunity on May 3.
Healthcare providers have found that in severe cases of COVID-19, patients have had high proinflammatory cytokines, indicating that the host immune system (cellular) is involved in the pathogenesis of SARS-CoV-2. Over the past few months, studies have suggested varying degrees of humoral immunity involvement in COVID-19. Yet, relatively little is known about the protective immune responses induced by SARS-CoV-2.
To address this gap in knowledge, the researchers from China sought to characterize the specific SARS-CoV-2 antibody and T-cell responses in COVID-19 patients. They compared the immune responses of 14 convalescent COVID-19 patients with those of six healthy individuals. Of the COVID-19 patients, eight were newly discharged and six were two weeks postdischarge.
Investigating humoral immune responses
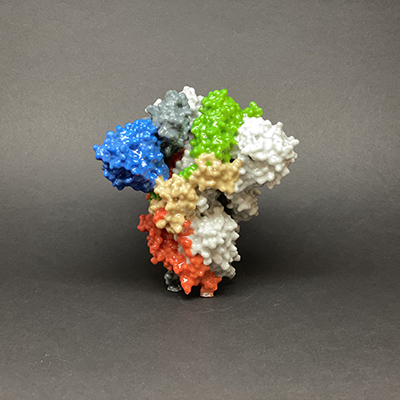
Blood samples were analyzed for levels of immunoglobulin M (IgM) and immunoglobulin G (IgG). The antiviral immune responses (IgM, IgG) against the SARS-CoV-2 nucleocapsid protein (NP) (which encapsulates the viral genome RNA), the S protein of the receptor-binding domain (S-RBD) (which binds to receptors on host cells), and the main protease antigens (critical for viral replication) were tested in a recombinant system.
The COVID-19 patients had high levels of IgG and IgM responses to SARS-CoV-2 proteins and could maintain IgG amounts for at least two weeks after discharge. The IgG responses were further characterized as being primarily IgG1 isotype in some cases and IgG3 in others.
Next, a pseudovirus particle-based neutralization assay against the SARS-CoV-2 S protein revealed that newly discharged patients had high neutralizing antibody titers indicative of a strong humoral immune response. These neutralizing antibodies prevent infectious particles from interacting with host cells. Follow-up patients also had neutralizing antibody titers.
Investigating cellular immune responses
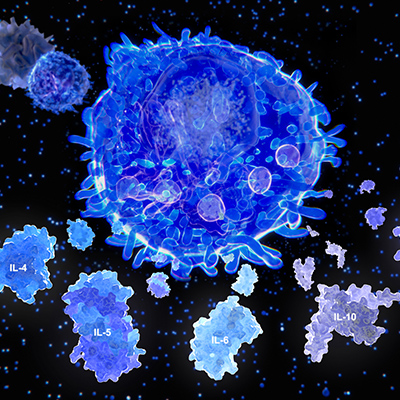
To explore cellular immune responses to SARS-CoV-2, the researchers isolated peripheral blood monocytic cells and analyzed them by flow cytometry. Generally, there were no significant differences in terms of T cells among COVID-19 patients and healthy donors. In some COVID-19 patients, high levels of interferon gamma (IFN-γ)-secreting NP-specific T cells suggest that those patients developed SARS-CoV-2-specific T-cell responses. This was observed in the same patients who had high concentrations of neutralizing antibodies.
Furthermore, IFN-γ-secreting S-RBD-specific T cells were detected at lower levels but in more patients than NP- or main protease-specific T cells. Three patients did show detectable levels of main protease-specific T cells. Only one patient showed high concentration of specific T cells to all three types of SARS-CoV-2 proteins. The follow-up patients did not show high levels of T cells, which suggests that antiviral T cells may not be maintained in high numbers in recovered patients.
Interestingly, the authors noted a positive correlation between the development of neutralizing antibodies and the activation of antiviral T cells; therefore, viral clearance may require collaborative humoral and cellular immune responses.
"Our results suggest that S-RBD is a promising target for SARS-CoV-2 vaccines," said co-senior study author Fang Chen, PhD, of Chui Yang Liu Hospital affiliated to Tsinghua University, in a statement. "But our findings need further confirmation in a large cohort of COVID-19 patients."
Do you have a unique perspective on your research related to virology or immunology? Contact the editor today to learn more.
Copyright © 2020 scienceboard.net