December 7, 2022 -- A small molecule KRASG12D inhibitor has triggered complete responses in preclinical pancreatic cancer models, raising hopes that the approach can improve outcomes in the hard-to-treat tumor type.
Pancreatic cancer is associated with poor outcomes, with the limited treatment options available today associated with a five-year survival rate of 11%. Almost 90% of the cancers are driven by mutations in the KRAS gene, a common oncogene that was considered undruggable until recently. The approval of Amgen's Lumakras (sotorasib) in non-small cell lung cancer showed it is possible to drug KRAS, but that molecule hits a mutation, G12C, that is only expressed by around 2% of pancreatic tumors.
G12D mutations are more common in pancreatic cancers, being found in around 36% of patients. The prevalence of the mutations led researchers at Penn Medicine's Abramson Cancer Center to study the effect of MRTX1133, a KRASG12D inhibitor in development at Mirati Therapeutics, in pancreatic cancer models.
The Penn team reported their findings December 6 in the journal Cancer Discovery. After validating the specificity and potency of the small molecule in vitro, the researchers tested the candidate in pancreatic ductal adenocarcinoma models with an intact immune system. The in vivo tests linked MRTX1133 to deep tumor regressions, including complete or near-complete remissions after 14 days, and raised hopes for the program.
"The results of this study are in stark contrast to anything we've seen before in pancreatic cancer," Dr. Ben Stanger, PhD, co-corresponding senior author and director of the Penn Pancreatic Cancer Research Center, said in a statement. "Even in preclinical research models for this cancer type, most drugs tested within the last decade -- including novel immunotherapies -- have had limited impact."
Studies of KRASG12C inhibitors and other targeted therapies suggest that tumors will develop resistance to MRTX1133. However, the Penn paper's assessment of the immune response after administration of the small molecule offers encouragement that the candidate can trigger durable responses.
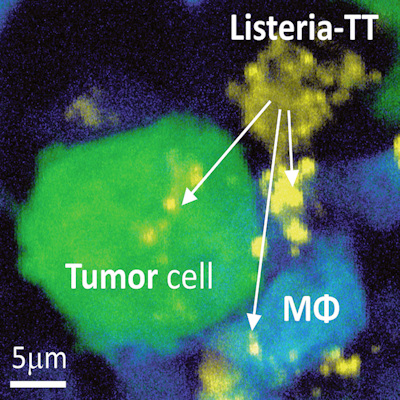
As well as cancer cell death, the researchers saw changes in the tumor microenvironment involving fibroblasts, matrix, and macrophages. The study found T cells were necessary for MRTX1133 to have its full antitumor effect. All complete remissions were accompanied by T cell mediated antitumor immunity. Depleting T cells accelerated tumor regrowth after therapy.
Based on the immune system changes, MRTX1133 may work synergistically with immunotherapies to improve the long-term response to treatment and stop the cancer from returning. Mirati has seen "increased activity" when the candidate is "combined with rational combination approaches" and is nearing the start of clinical development.
"After many years of work to find much-needed new approaches for patients with pancreatic cancer, it's exciting to have a new class of drugs on the horizon," said co-corresponding author Dr. Robert Vonderheide, director of the Abramson Cancer Center. "We're optimistic that KRAS G12D inhibitors will make their way into clinical trials soon. KRAS is surrendering, and now we know the immune system can see it."
Copyright © 2022 scienceboard.net