February 11, 2020 -- Immune cells may be better at sensing each other than previously thought, according to a new study published in Immunity on February 11. Researchers from Germany, the Netherlands, and the U.K. revealed a mechanism T cells use to work as a team and mutually determine how to fight infections.
When faced with an infection, T cells normally follow a remarkably reproducible response pattern of expansion, contraction, and memory formation. Population-intrinsic and -extrinsic regulation of T cells occur but are not mutually exclusive. Conventional T-cell response is often measured by extrinsic signals, such as those sent by regulatory T cells or dendritic cells, which can be variable and thus difficult to use to infer population size. Alternatively, if a population of T cells mutually controls each other, then the strength of regulatory signals scales with population size in an intrinsic manner.
But there is not much information regarding specific intrinsic control mechanisms. One previously described mechanism, bacterial quorum regulation, can be used as a prototype for population-intrinsic behavior in T cells. In this scenario, members of the population sense each other and adjust their behavior accordingly to strike a balance between rapid expansion and preventing excessive self-damaging reactions.
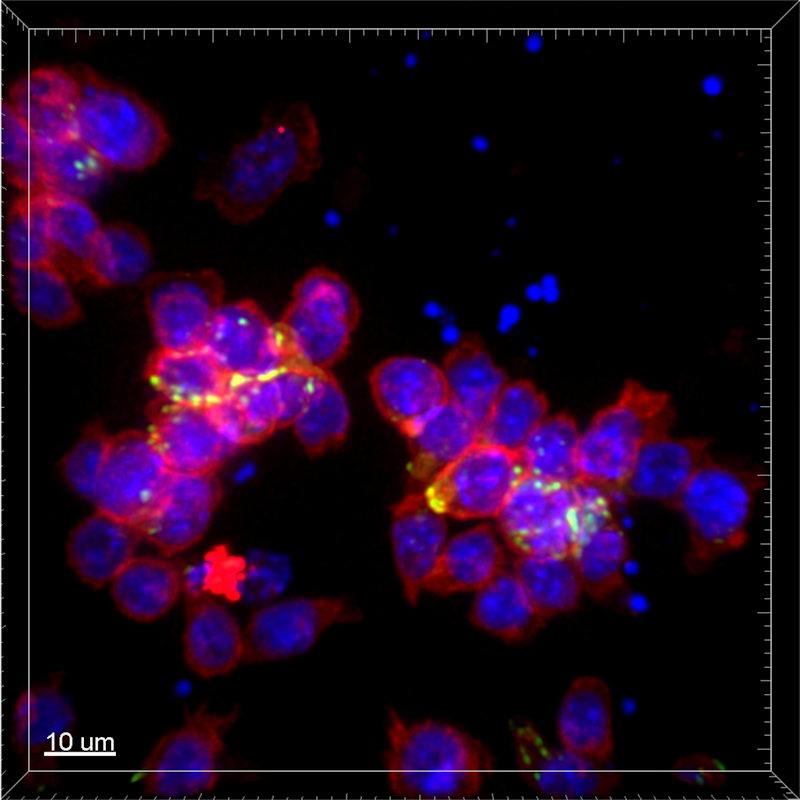
In the current study, the researchers used time-lapse microscopy, genetic perturbation, bioinformatic predictions, and mathematical modeling to investigate if CD8+ T cells use quorum regulation to control their population dynamics.
Cooperative immune cells
"We showed that these immune cells perceive and regulate each other. The immune cells act as a team and not as autonomously acting individualists," said Dr. Jan Rohr, head of the study and a scientist at the University Hospital of Freiburg Centre for Immunodeficiency, in a statement. "This principle of density control of immune cells is simple and very effective. This makes it reliable and at the same time hopefully accessible for therapeutic approaches."
The researchers found that activated T cells mutually promote their expansions when they are present at low densities, but they also limit further proliferation once sufficient numbers have been reached. This mechanism leads to efficient amplification of initial immune reactions and also prevents potentially dangerous immunopathologies.
Specifically, CD28 and IL-2 induced CD80 expression by activated T cells, which could in turn bind to CD28 to augment IL-2 production. This positive feedback loop perpetuated T-cell expansion. However, at some point it becomes necessary to limit this amplification. This is accomplished through a negative feedback circuit acting via CTLA-4, by blocking ligand binding of CD28 and IL-2. This evidence supports a mechanistic explanation of how T-cell population dynamics are regulated in a cell density manner by receiving signals from a variety of cell types.
These new findings shed light on immunotherapy dynamics. Traditionally, therapies contain high cell counts to ensure effectiveness. However, "it is possible that the immune cells switch off each other if they are administered at high numbers. A repeated administration of lower numbers of immune cells may fight the tumor cells more effectively," Rohr said. The extent to which this might help to improve current immunotherapies will have to be investigated in further studies.
Do you have a unique perspective on your research related to immunology? Contact the editor today to learn more.
Copyright © 2020 scienceboard.net






