June 30, 2021 -- Scientists are identifying key factors that aid in the effectiveness of oncolytic viruses during the treatment of cancers, which could lead to better immunotherapies and inform clinicians which patients might benefit from the treatment. Findings from a June 22 Nature Communications article point to the clinical relevance and underlying mechanisms of a novel anticancer treatment.
Oncolytic viruses can selectively replicate in tumor cells, destroying them without causing harm to normal healthy tissues. As such, many of these "good" viruses are under clinical investigation against various types of cancers. Despite their clinical potential, the use of oncolytic viruses as a standalone therapy is often ineffective due to incomplete tumor regression.
The efficacy of oncolytic virus treatments can be improved with the use of synergistic modalities, for example combinations with other forms of immunotherapy like checkpoint inhibitors, or by treating patients whose genetic characteristics are favorable to the virus life cycle and would most likely benefit from the treatment.
However, to reach the point of rational design of combination treatments, researchers must first achieve a better understanding of the oncolytic virus life cycle and host cellular determinants that contribute to virus infection.
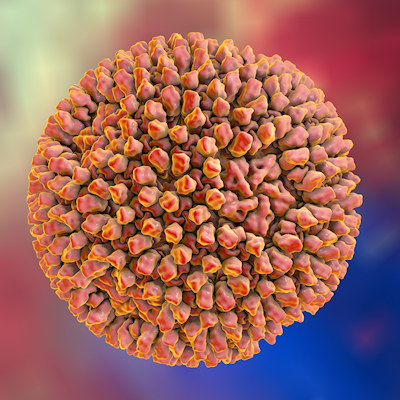
Researchers from the Laboratory of Oncolytic-Virus-Immuno-Therapeutics (LOVIT) in the department of oncology at the Luxembourg Institute of Health were interested in learning more about rat protoparvovirus (H-1PV), which is a clinically relevant oncolytic virus with demonstrated preclinical and clinical antitumor efficacy.
H-1PV is a small, nonenveloped, single-stranded DNA virus whose replication and gene expression are dependent on many host cell factors. While some of these factors have been identified, many remain undetermined. Moreover, it is unknown why some cancer cell lines are highly susceptible to H-1PV infection, and others are less sensitive or even completely refractory.
The extracellular matrix is often a barrier to a virus on its way into the host cells, and some viruses have developed strategies to bind specific extracellular matrix components, leading to a large quantity of viral particles at the host cell surface to ensure engagement with host receptors. This attachment is therefore an essential event that primes the virus infection. For H-1PV, it is known that sialic acid is needed for cell attachment, but the attachment receptor is still unknown.
"In this context, we sought to elucidate the features of host cancer cells that enable oncolytic viruses to effectively infect and destroy them, focusing specifically on the factors required for cell attachment and entry," said Antonio Marchini, PhD, senior author and leader of LOVIT, in a statement.
Using siRNA to learn about oncolytic virus cell attachment
Using high-throughput RNA interference screening to identify host factors involved in the oncolytic H-1PV life cycle, the researchers systematically "turned off" close to 7,000 genes of cervical carcinoma cells to analyze their effect on H-1PV infectivity. They identified 151 top activator genes and 89 genes that acted as repressors.
These genes were then screened for association with sialic acid, indicating association with the host cell surface. The activator proteins associated with the cell surface were then grouped into protein classes based on cellular processes.
The researchers focused their analysis on two extracellular matrix genes and seven transmembrane signal receptor genes. They were particularly interested in the LAMC1 extracellular matrix gene, which encodes the laminin γ1 chain. Laminins are glycosylated proteins rich in sialic acid residues.
When LAMC1 expression was silenced, the researchers found that viral cell binding and entry were decreased. Cells that were transduced with LAMC1 small interfering RNA (siRNA) were significantly more resistant to H-1PV cytotoxicity.
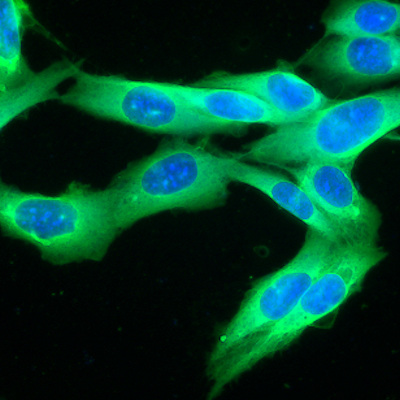
To further determine if H-1PV interacts with laminins at the cell surface, the researchers colocalized H-1PV with laminins and conducted confocal analysis, which showed that the virus was often associated with laminins. The researchers also confirmed that the laminins involved with H-1PV cell attachment were laminin γ1 encoded by LAMC1 and not other members of the laminin family.
With this battery of tests, the scientists confirmed the importance of laminin γ1 in mediating virus cell attachment and penetration. Similarly, the team found that silencing the LAMB1 gene encoding the laminin β1 protein led to a decrease in H-1PV cell binding and entry.
"Essentially, laminins at the surface of the cancer cell are the 'door' that allows the virus to recognize its target, attach itself and penetrate into it, subsequently leading to its destruction," explained Amit Kulkarni, PhD, first author and postdoctoral researcher at LOVIT. "In particular, the virus interacts with a specific portion of the laminin, a sugar called sialic acid, which is essential for this binding and entry process and for infection."
Importantly, the authors noted that interactions with laminins and other extracellular matrix constituents seem to be a common mechanism conserved throughout the evolution of different classes of microbes. This points toward the relevance of the results for not only H-1PV but other oncolytic viruses.
Implications of laminins for cancer treatments
In different types of tumors, the team found that LAMC1 and LAMB1 are statistically associated with poor patient survival. By analyzing expression patterns of laminin γ1 in human biopsies, the scientists found that laminins γ1 and β1 were overexpressed in pancreatic carcinoma and glioblastoma cells compared to healthy tissues. Screening different tumor types, they also found that 36 cancer cell lines of various origin were highly susceptible to H-1PV infectivity.
"These observations indicate that elevated laminin expression is associated with poor patient prognosis and survival in a variety of tumors, including gliomas and glioblastoma," Marchini added. "The encouraging fact, however, is that cancers displaying high laminin levels are more susceptible to being infected and destroyed by the H-1PV virus and that patients with these tumors are therefore more likely to be responsive to this therapy."
According to the authors, the information revealed by the study could lead to the classification of cancer patients according to their laminin expression levels to predict their responsiveness to H-1PV-based anticancer therapies. This would enable more efficient clinical trials and ultimately enhance the development of combinatorial cancer treatments.
Do you have a unique perspective on your research related to immuno-oncology? Contact the editor today to learn more.
Copyright © 2021 scienceboard.net