August 3, 2020 -- A new research study used whole-genome sequencing to analyze the genetic profile of patients with the SARS-CoV-2 virus to gain more insight into how it turns the body's own immune system against itself. The findings could help researchers develop drugs to target the virus, according to an August 3 report in Nature Medicine.
Researchers focused on how SARS-CoV-2 attacks pathways in the body's complement and coagulation systems. The complement system is part of the immune system and enhances the ability of antibodies and phagocytic cells to clear microbes, promote inflammation, and attack a pathogen's cell membrane, while the coagulation system includes cells, proteins, and processes that mediate blood clotting and are crucial to controlling pathogenesis associated with infections.
While both systems have evolved to help the body deal with a viral invader or injury, when they do not function properly, they can contribute to inflammation and disease. For example, the complement system can cause excessive inflammation when dysregulated. Therefore, virally encoded structural mimics of complement and coagulation factors may contribute to coronavirus-associated immune-mediated pathogenesis.
"The new coronavirus -- by mimicking complement or coagulation proteins -- might drive both systems into a hyperactive state," said lead author Sagi Shapira, PhD, MPH, from Columbia University Vagelos College of Physicians and Surgeons, in a statement.
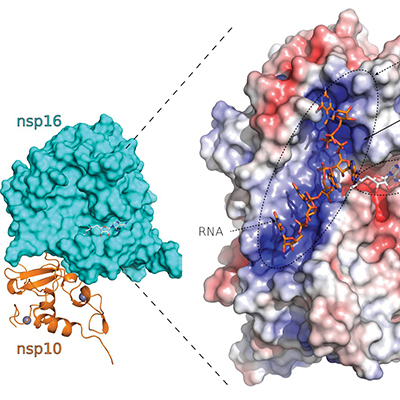
In a previous study, researchers from Columbia University Irving Medicine Center mapped over 140 cellular proteins that are structurally mimicked by coronaviruses and identified targets of the complement system.
"Viruses have proteins that can mimic certain host proteins to trick the host's cells into aiding the virus with completing its life cycle," Shapira said. "Beyond the fundamental biological questions that we were interested in addressing, based on our previous work and the work of others, we suspected that identifying those mimics could provide clues about how viruses cause disease."
Complement and coagulation as indicators of SARS-CoV-2 susceptibility
In a retrospective observational study of 11,116 patients with SARS-CoV-2, the researchers found that age-related macular degeneration (a proxy for complement-activation disorders) and coagulation disorders (thrombocytopenia, thrombosis, and hemorrhage) are risk factors for SARS-CoV-2-associated disease. They found that hyperactive complement and coagulative states predispose individuals to adverse outcomes associated with SARS-CoV-2 infection.
"We found that complement is one of the most differentially expressed pathways in SARS-CoV-2 infected patients," said author Nicholas Tatonetti, PhD, from Columbia University Vagelos College of Physicians and Surgeons. "As part of the immune system, you would expect to see complement activated, but it seems over and above what you'd see in other infections like the flu."
Whole-genome RNA sequencing profiles were used to identify differentially regulated genes and pathways in 650 nasopharyngeal swabs (control and SARS-CoV-2 infected). In addition to immune factors such as type I interferons and dysregulation of interleukin-6-dependent inflammatory responses, transcriptional control of complement and coagulation cascades was identified as a feature of SARS-CoV-2 infection.
Dysfunction of the complement and coagulation cascades can result from acquired dysregulation, genetically encoded variants, or both. The researchers conducted a study to evaluate if 102 genes with known roles in regulating complement or coagulation cascades were associated with poor SARS-CoV-2 clinical outcomes. The team identified 11 loci across seven genes, including a mutation in coagulation factor III and 10 variants associated with age-related macular degeneration, as potential genetic markers of SARS-CoV-2 disease outcomes.
The researchers repeated the study and reproduced six of the 11 previous findings and identified 16 additional loci. Five variants were associated with α-2-macroglobulin, a regulator of fibrin clot formation and inflammatory cascades. Moreover, a mutation on COLEC11, a gene for a protein that binds carbohydrate antigens on viruses to facilitate their recognition and removal, is associated with poor clinical outcomes. The researchers suggested that sugar moieties on viral proteins may serve as antigenic targets of immunological responses to SARS-CoV-2 infection. However, experimental validation of this hypothesis is needed.
Exploring treating COVID-19 with anticoagulation drugs
The authors noted that physicians treating COVID-19 patients have noticed coagulation issues since the outbreak of the pandemic. Now, several clinical trials are exploring the use of preexisting anticoagulation treatments in COVID-19 patients. As a less well-known therapy, complement inhibitors are used primarily in the treatment of rare disease, however at least one clinical trial is exploring their use for COVID-19.
"I think our findings provide a stronger foundation for the idea that coagulation and complement play a role in COVID," Tatonetti said. "[This] will hopefully inspire others to evaluate this hypothesis and see if it's something that can be useful for fighting the ongoing pandemic."
Do you have a unique perspective on your research related to virology or immunology? Contact the editor today to learn more.
Copyright © 2020 scienceboard.net